Examining the Cuyahoga Overdose Surveillance Quarterly Data: Why Fewer Deaths Doesn’t Mean the Crisis Is Over
Cuyahoga County has reported a significant decline in overdose deaths. At first glance, this appears to be a clear indicator of progress. Fatalities dropped sharply at the end of 2025, and emergency department visits for suspected overdoses also decreased. For a region that has long been defined by the severity of the overdose crisis, these trends suggest measurable improvement. However, it is critical to distinguish between improvement and resolution.
A reduction in deaths does not necessarily mean that the underlying crisis has been solved. Instead, it may indicate that the conditions producing harm are being managed more effectively, not eliminated. This distinction is essential for understanding the current moment. Although fewer individuals are dying, the structural vulnerabilities that contribute to overdose risk remain largely unchanged. Economic instability, limited access to healthcare, untreated trauma, and the criminalization of substance use continue to shape the environment in which this crisis exists. As a result, the decline in deaths should be interpreted as a shift in outcomes, not a disappearance of risk.
For nearly a decade, fentanyl has been the primary driver of overdose mortality. Its potency significantly increased the lethality of the drug
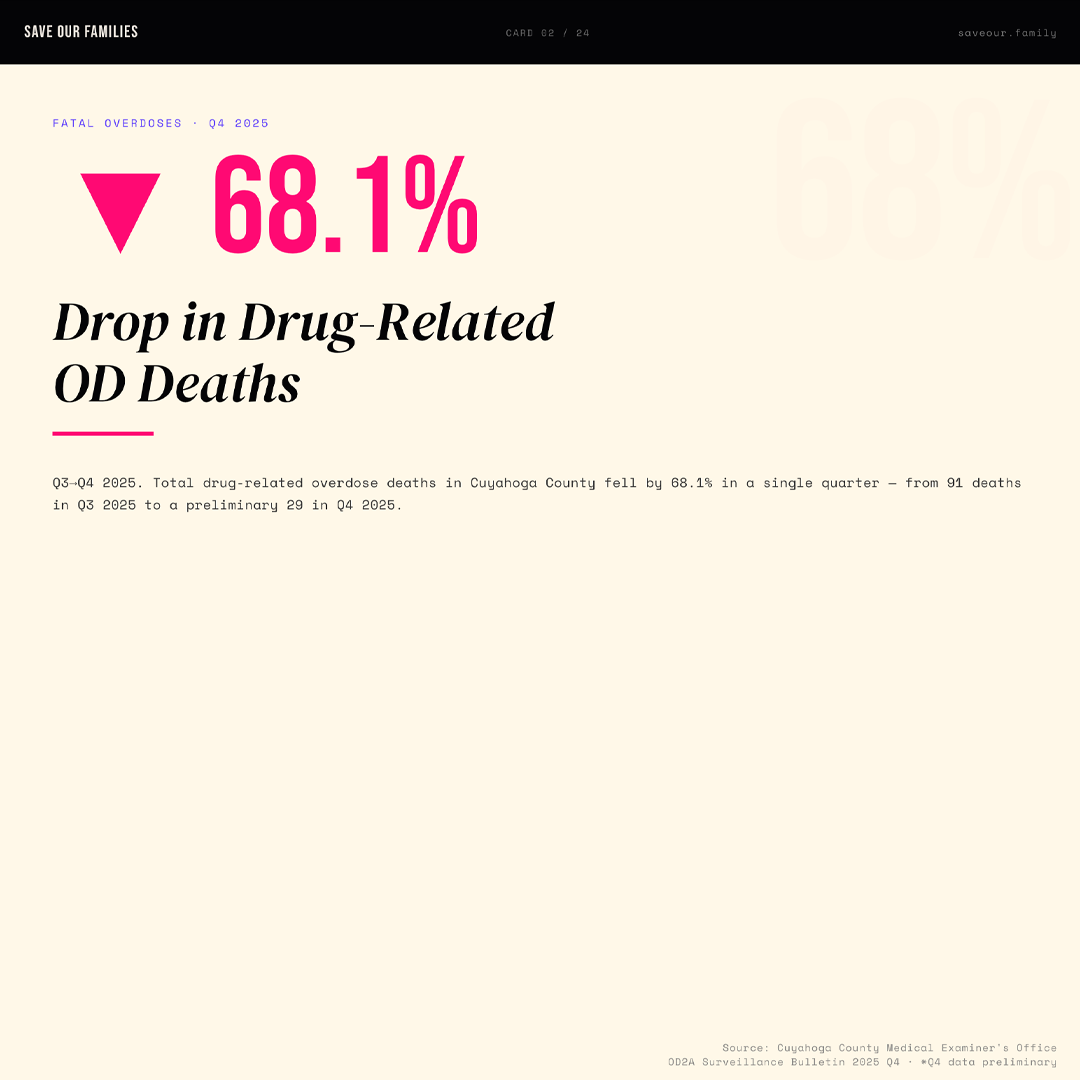
supply, overwhelming both individuals and public health systems. Recent data suggests that fentanyl-related deaths are decreasing, contributing to one of the lowest projected annual death totals since its widespread emergence in the mid-2010s. Yet, public health crises rarely end when a single contributing factor declines. Instead, they evolve.
Current surveillance data indicates that the drug supply is becoming more complex rather than less dangerous. Cocaine has emerged as the most frequently identified substance in laboratory testing, surpassing fentanyl. At the same time, non-opioid sedatives such as medetomidine and xylazine are appearing more frequently. These substances introduce new challenges because they do not respond to naloxone, the primary medication used to reverse opioid overdoses. This shift represents a structural change in the nature of overdose risk. It requires a reassessment of existing intervention strategies, many of which were designed primarily to address opioid-related harm.
Despite this increasing complexity, overdose deaths are declining. This apparent contradiction can be explained by the expansion and effectiveness of harm reduction interventions. Harm reduction strategies, including naloxone distribution and community-based outreach, have reached a level of saturation that is influencing population-level outcomes. Although fewer naloxone kits are being distributed and administered, this decrease appears to reflect a reduced need for emergency reversal rather than a decline in service engagement.
In this context, harm reduction is functioning as intended. It does not eliminate risk but reduces the likelihood that risk results in death. This distinction is central to understanding its role in public health.
For many years, harm reduction has been debated as an ideological matter rather than evaluated on the basis of evidence. The current data challenges that framing. The decline in overdose deaths suggests that approaches centered on accessibility, trust, and immediate care are producing measurable results.
However, survival alone is not a sufficient outcome.
A critical development in the current data is the expansion of linkage-to-care systems. Increasingly, individuals who experience or are at risk of overdose are being connected to longer-term treatment options. These systems aim to bridge the gap between emergency intervention and sustained recovery, particularly for populations at high risk, such as individuals transitioning out of incarceration. This represents a shift away from earlier models of care, which were often reactive and episodic. Historically, overdose response focused on reversing the immediate crisis without ensuring ongoing support. The emerging model emphasizes continuity of care, recognizing that long-term stabilization requires sustained engagement.
Despite this progress, significant gaps remain. Not all individuals who are identified and engaged in care can initiate treatment, and not all who begin treatment remain connected over time. The gap between initial contact and sustained care continues to shape the crisis’s long-term trajectory.
This gap is particularly important because it highlights the limits of current interventions. While harm reduction can reduce mortality, it does not fully address the broader conditions that contribute to substance use and instability. At the same time, the decline in overdose deaths introduces new challenges for policy and resource allocation. When public health indicators improve, there is often pressure to reallocate funding or reduce investment in intervention strategies. However, the current decline is not the result of a fully transformed system. It reflects the impact of sustained intervention within a system that remains structurally unequal.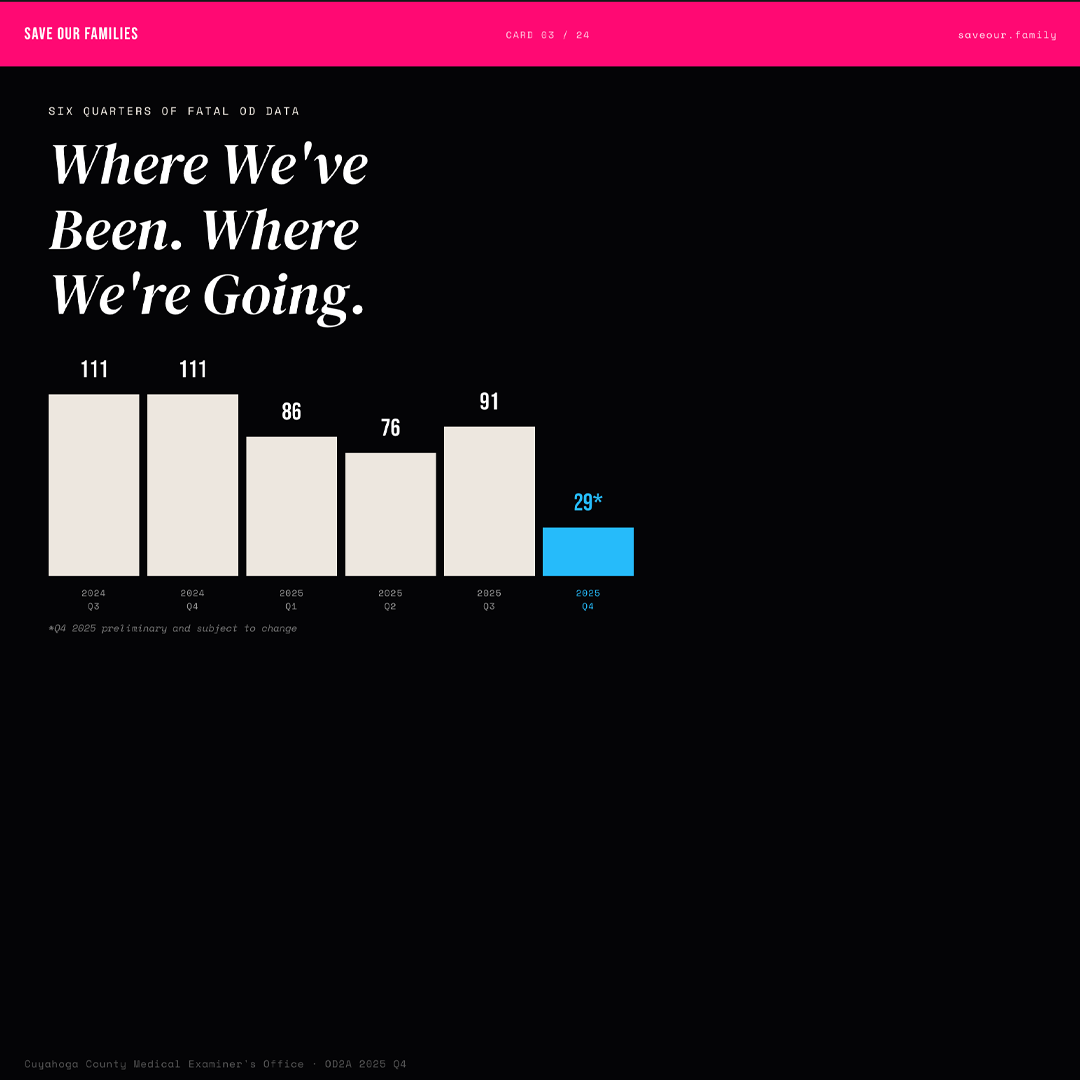 Reducing or withdrawing resources at this stage would risk reversing recent progress. The current improvements are contingent on continued investment and adaptation.
Reducing or withdrawing resources at this stage would risk reversing recent progress. The current improvements are contingent on continued investment and adaptation.
It is also important to recognize that the factors driving the crisis remain unresolved. They have been mitigated. Mitigation requires ongoing effort, monitoring, and responsiveness to emerging trends.
The current moment presents a critical opportunity. The data demonstrates that targeted, community-based interventions can reduce overdose deaths, even in the presence of persistent structural challenges. The key question is whether this evidence will be used to strengthen and expand these interventions or to justify scaling them back.
At Save Our Families, this period is understood as a transition rather than a conclusion. The focus moving forward must be on adapting to an increasingly complex drug supply, strengthening systems that connect individuals to care, and addressing the broader social and structural factors that contribute to vulnerability.
Equally important is resisting the assumption that progress will continue without sustained effort. Public health outcomes are not self-sustaining. They depend on ongoing intervention, evaluation, and investment. The decline in overdose deaths in Cuyahoga County is both real and significant. It should inform future strategy and guide decision-making. However, it should not lead to complacency. The true measure of success is not simply whether fewer people die in a given period. It is whether the systems that contribute to risk are being fundamentally changed.
Source: https://ccbh.net/overdose-data-dashboard/
about author
Created by the team at Save Our Families.
subscribe to our newsletter
Join the Save Our Families newsletter for updates on community care, mental health tools, healing stories, and events you won’t want to miss.
Note: We promise not to flood your inbox—just healing vibes, resources, and real talk.
Recent Posts
Examining the Cuyahoga Overdose Surveillance Quarterly Data: Why Fewer Deaths Doesn’t Mean the Crisis Is Over
Cuyahoga County has reported a significant decline in overdose deaths. At first glance, this appears to be a clear indicator of progress. Fatalities dropped sharply at the end of 2025, and emergency department visits for
When Bipolar Disorder Is Misread: A Call for Better Understanding and Support
A National Bipolar Day Editorial On any given day, someone is being labeled difficult, unpredictable, or unstable. A student was removed from class.An employee was written up for inconsistency.An individual in a courtroom is struggling
Save Our Families Launches Community Care & Leadership Series to Strengthen Prevention Through Skill-Based Education
Cleveland, Ohio – Save Our Families announces the launch of its Spring 2026 Community Care & Leadership Series, a four-week virtual educational program designed to equip community members with practical tools for intervention, dialogue, sustainability,